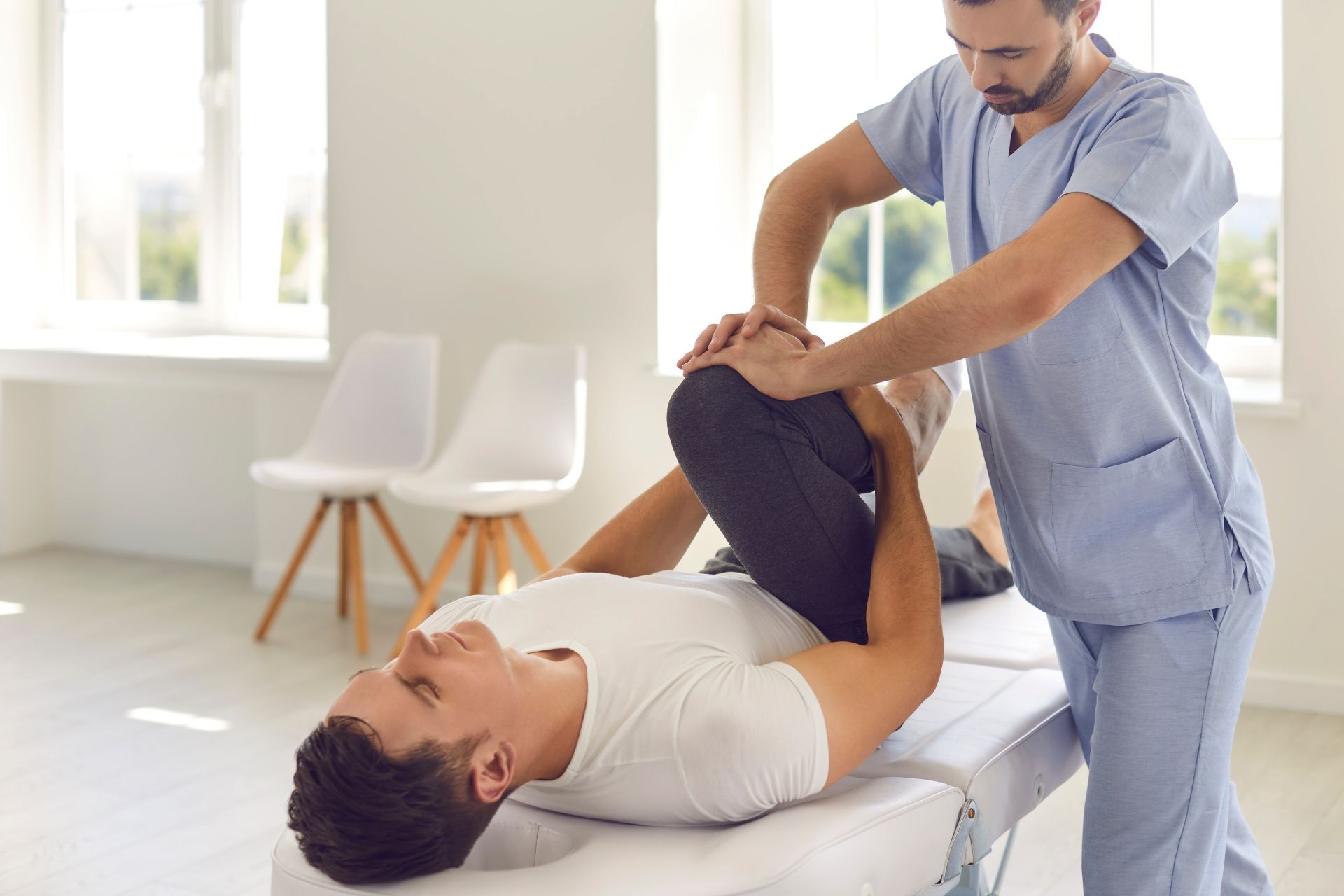
Ligament Stress Testing
How is ligament stress testing used to diagnose injuries in athletes?
Ligament stress testing is a valuable diagnostic tool used by healthcare professionals to assess injuries in athletes. By applying controlled stress to specific ligaments, such as the anterior cruciate ligament (ACL) or medial collateral ligament (MCL), clinicians can evaluate the stability and integrity of these structures. This testing helps identify any abnormalities or weaknesses in the ligaments, which can indicate the presence of a sprain, tear, or other injury that may require further evaluation or treatment.